 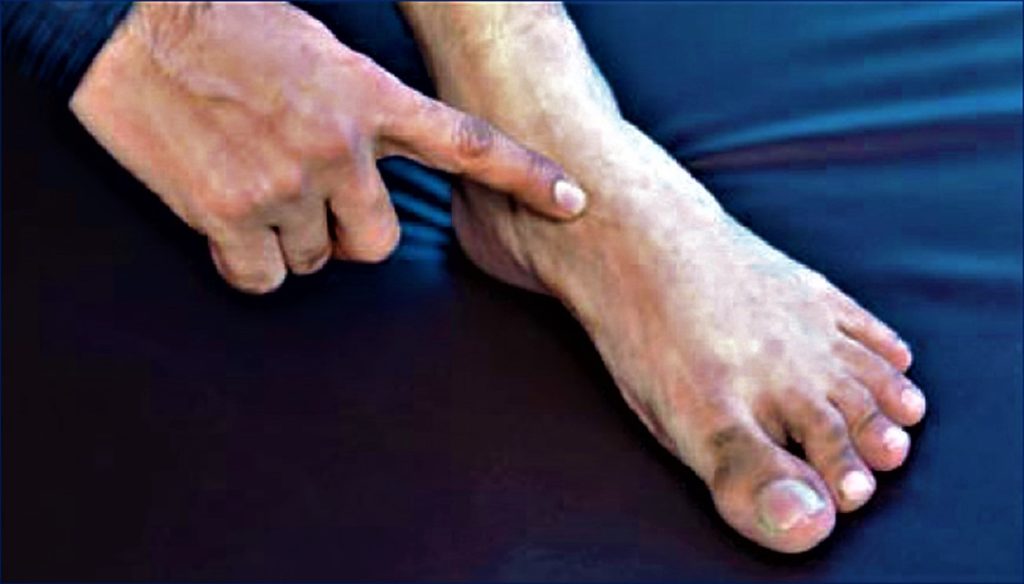 
Assessment of mid-foot mobility, standing and walking posture, and ability to and quality of hopįigure 5. Assessment of mid-foot motion – stabilising rear – foot and rotating forefootįigure 4. 1 The key features to examine include mid-foot posture for pronation ( Figure 2), mid-foot motion and stability ( Figures 3, 4) and palpation of the navicular ( Figure 5).įigure 3. For traumatic presentations and severe swelling, it is important to assess neurovascular structures and the possibility of compartment syndrome. From a patho-anatomical diagnostic basis, careful systematic palpation, clarifying the site of tenderness is key to assessment of the likely pain generator. The range of mid-foot mobility provides a feel for stiffness or hypermobility. In gradual-onset conditions, activity and loadings, progression and current functional limitations, and previous treatment are important.Įxamination involves review of foot type biomechanically by observing foot posture on standing. History in acute injury requires clarifying precise details of mechanism and subsequent functional deficit in terms of the ability to weight-bear, and swelling and bruising. Clinical assessmentĪs in all areas of general practice, the approach to clinical assessment involves review in terms of what is likely in this person, at this age, in this region, doing this activity, and what must not be missed (red flags). Complex rotations and flexion-extensions fulfil these roles. Together, these anatomical structures contribute to the integrity of the longitudinal and transverse arches of the foot, which are critical for shock absorption at foot strike (foot landing in supination), energy store in stance and propulsion at heel lift-off. Joint, bone and tendon insertion pathology, especially in the immature skeleton apophyses in these tissues, need to be included in the diagnostic mix of pain in the mid-foot region. Structures immediately adjacent include the bases of the metatarsals. The main players include the navicular bone and the three cuneiform bones medially and the cuboid laterally, the proximal tarsal and the distal tarso-metatarsal joints, the ligaments, including the central (anterior cruciate ligament equivalent) first tarso-metatarsal ligament 3 and medial spring ligament, tibialis anterior and posterior and peroneal tendons. 1 However, from a differential diagnosis assessment perspective, it is necessary to consider conditions of significance occurring at the margins of the more strictly applied anatomical boundaries. Bony anatomy of the foot – relationship of mid-foot bones to metatarsals and proximal tarsal bonesĪnatomically, the mid-foot is the region distal to the talus and calcaneus, and proximal to metatarsal bases ( Figure 1). Recent trends in imaging and medical management will be outlined. 1 The aim of this article is to provide some guidance in recognising and managing red flag conditions in this region. Delay in diagnosis has a potentially adverse impact on outcome. However, there is a clustering of diagnoses occurring in the mid-foot region, including navicular bone stress, Lisfranc ligament disruption and tibialis posterior dysfunction, that require sound management. Unfamiliarity arising from infrequent presentations adds to management difficulties in the primary care setting. 
Overall in general practice presentations, acute and overuse mid-foot conditions may not be encountered frequently. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
